Macular Pucker (Epiretinal Membrane) Diagnosis and Treatment in Sarasota, FL
Macular pucker is treatable, and vision often improves with the right treatment.
Macular pucker is a common condition in adults over 50 where a thin layer of scar tissue forms on the surface of the retina and gently wrinkles the macula. This can cause straight lines to look wavy, words to appear distorted, or vision to seem mildly blurred in one eye.
Our ophthalmologists specialize in diagnosing macular pucker and offering careful observation and advanced surgical treatment when needed.
What Is Macular Pucker?
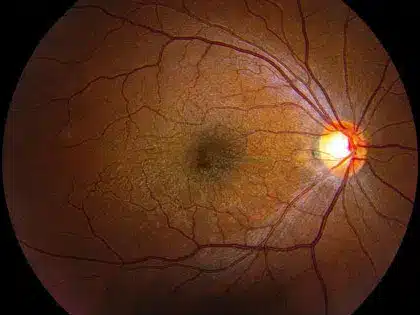
Macular pucker is a common condition that affects the central portion of the retina, known as the macula. A macular pucker occurs when a thin membrane on the surface of the retina pulls the macular layers out of position, causing blurring and distortion of vision. This condition goes by several names, including a retinal wrinkle, epiretinal membrane, and cellophane maculopathy.What Causes Macular Pucker?
To answer this question, a lesson in eye anatomy is required. The retina is a thin layer in the back of the eye that receives light and changes those images to signals for the brain. Directly in front of the retina, filling the eye is the vitreous jelly. When light enters the eye, it passes through the cornea, lens, and vitreous jelly to be focused on the center of the retina, known as the macula.Throughout the first 50-70 years of life, the vitreous jelly is attached to the surface of the macula. As the eye ages, the vitreous begins to separate from the surface of the retina, leaving behind small bunches of cells on the macula. These cells act like scar tissue, spreading themselves out into a sheet-like membrane. The membrane eventually contracts, putting tension and causing wrinkles to the surface of the retina.
While epiretinal membranes are extremely common in patients >50 years old, they are not part of the normal eye anatomy. Although most epiretinal membranes form spontaneously (without the patient’s input), there are some risk factors that may increase the chances of macular pucker formation. These risk factors include diabetes, eye trauma, surgery, bleeding, inflammation, retinal tear, or retinal laser.
Is Macular Pucker Inherited?
While there are surely some inherited factors that contribute to macular pucker formation, no particular genetic focus has been implicated in the development of a retinal wrinkle. Most epiretinal membranes form spontaneously regardless of family or personal history. Unfortunately, you cannot use exercise, nutrition, or medicine to avoid a macular pucker. Retina specialists consider macular pucker to be a fact of life given the anatomy and physiology of the human eyeball.
What are the Symptoms of a Wrinkle in the Retina?
When the membrane pulls hard enough to shift the position of the light-sensing cells in the retina, called photoreceptors, the epiretinal membrane becomes symptomatic. Depending on whether the photoreceptors are shifted closed together or farther apart will determine whether the patient experiences magnification or minification of images. Sometimes the retinal wrinkle is irregular, causing distortion or just plain blurry vision. Pain is not associated with macular pucker.
If the ophthalmologist is unsure of the source of the macular edema, he may order additional images with a camera technology called fluorescein angiography. This test involves injecting dye into an arm vein and taking pictures at it flows through the retinal vessels. Any swelling withing the macula glows brighter as the test progresses, sometimes revealing the source of the leakage.
How is an Epiretinal Membrane Diagnosed?
If you are experiencing a distortion of vision and suspect that you may have a wrinkle in your retina, it is advisable to seek a dilated exam with an ophthalmologist specialized in macula and retina disease. During this visit, you will have your vision checked, eye pressure measured, and pupils dilated.
The ophthalmic technician will then take a specialized image of your retina called an optical coherence tomograph (OCT). The OCT is capable of imaging the macula down to a hundredth of a millimeter by sending slices of infrared light through the pupil. This camera is so sensitive that it often catches epiretinal membranes that the patient didn’t even know were there.
Following retinal imaging, the retina doctor will then review your images, examine your eye, and discuss the findings and risks/benefits to treatment.
What Can Be Done to Treat Macular Pucker?
Most epiretinal membranes are mild with minimal blurring or distortion of vision. In addition, macular pucker doesn’t progress quickly or lead to immediate irreversible vision loss. For these reasons, the majority of retinal wrinkles are observed without treatment. Most patients do not experience progression of their epiretinal membrane or blurriness even years after the initial diagnosis.
In patients with symptomatic macular wrinkling, a retinal surgeon may suggest surgical removal of the epiretinal membrane. This procedure is performed at an outpatient surgical center under local anesthesia, similar to cataract surgery. During the surgery, the ophthalmologist removes the vitreous jelly that fills the eye, a process known as vitrectomy. After the jelly is removed, microscopic tweezers are used to peel the membrane off of the surface of the macula. This 30-minute surgery is painless and curative for macular pucker.
Restrictions Following a Vitrectomy
There are minimal restrictions following a vitrectomy. Patients typically wear a patch overnight. They are examined in the ophthalmologist’s clinic one day later, one week later, and one month later. Drops are used for one month to prevent infection and inflammation. Repeat macular imaging demonstrates how the retina is returning to its pre-wrinkled state as the weeks and months go by.
The vision is expected to be back to pre-operative clarity by the end of the first week. The vision continues to improve up to one year after surgery, with most patients reporting reduced distortion and gaining additional lines on the eye chart. While most patients report an improvement in their visual symptoms, it is common for them to also report a small amount of residual distortion from the fact that the membrane was there in the first place.
The biggest risk to membrane peel surgery is retinal detachment, which occurs in 2% of cases weeks or months after surgery. In addition, patients who have not previously undergone cataract surgery will develop a cataract within 1-2 years following a vitrectomy.
Does the Wrinkle in the Retina Ever Reoccur?
It is unlikely, but still possible for macular pucker to recur. One reason for recurrence is incomplete removal during the original procedure. A surgeon may intentionally leave some membrane in the peripheral macula to avoid the risk of instrument trauma during the procedure. In other cases, the wrinkle may reform due to ongoing inflammation or other healing response from the eye.
Fortunately, surgeons can reduce the risk for recurrence by not only peeling the epiretinal membrane but by peeling the layer directly beneath it, called the internal limiting membrane (ILM). Patients can help reduce recurrence by using their anti-inflammatory drops as prescribed after surgery.
If an epiretinal membrane recurs, the treatment options are the same. If visual symptoms are minimal, the macular pucker can be safely observed. If the visual declines, a repeat vitrectomy, and membrane peel may be performed.
Macular Pucker FAQs
What is a macular pucker?
A macular pucker is a thin layer of scar tissue that forms on the surface of the macula and wrinkles the central retina. This can cause distortion or mild blurring in the center of your vision.
The macula is responsible for sharp, detailed sight used for reading and recognizing faces. When scar tissue, also called an epiretinal membrane, forms and contracts, it pulls on the macula and creates a wrinkled or puckered appearance.
Macular pucker is most common in adults over age 50 and often develops as part of normal aging. It usually affects one eye and does not cause pain.
What causes macular pucker?
Macular pucker is most commonly caused by normal age-related changes inside the eye. As the vitreous gel naturally shrinks and separates from the retina over time, it can leave behind microscopic cells on the surface of the macula. These cells gradually form a thin scar-like membrane that contracts and wrinkles the retina.
This process is usually part of normal aging and is not something patients cause through lifestyle or activity. In most cases, macular pucker develops spontaneously without a specific trigger.
Less commonly, macular pucker can occur after:
- Retinal tears or retinal detachment
- Eye surgery, including cataract surgery
- Eye inflammation
- Diabetes
- Trauma to the eye
When these conditions irritate the retina, the healing response can lead to scar tissue formation on the macula. Over time, that scar tissue may tighten and cause distortion of central vision.
Is epiretinal membrane the same as macular pucker?
Yes, an epiretinal membrane and a macular pucker refer to the same condition. “Epiretinal membrane” is the medical term, while “macular pucker” is the more common patient-friendly name.
An epiretinal membrane is a thin layer of scar tissue that forms on the surface of the macula. As this membrane contracts, it gently wrinkles or puckers the retina, which can distort central vision. That wrinkling effect is what gives the condition its name, macular pucker.
Both terms describe the same process and the same treatment options. When symptoms become significant, surgical removal of the membrane can reduce distortion and improve visual clarity.
What does vision look like with macular pucker?
Vision with macular pucker often appears distorted or slightly warped in the center. Straight lines may look wavy, letters may seem uneven, and objects can appear mildly stretched or compressed.
Many patients notice difficulty reading small print or feel that words are missing or bent in the middle of a sentence. Some describe a blurry or gray area in central vision, while others notice that faces look subtly distorted. Peripheral vision is typically unaffected.
In mild cases, the distortion may be subtle and stable for years. In more advanced cases, tightening of the scar tissue can increase distortion and reduce clarity. Covering one eye at a time can help reveal changes that may not be obvious when both eyes are open.
How serious is a macular pucker?
Macular pucker is usually not an emergency and does not cause sudden blindness, but it can significantly affect central vision over time. The seriousness depends on how much the scar tissue is distorting the macula and how much it interferes with daily activities.
In many patients, macular pucker is mild and stable. Vision may be slightly distorted but still functional for reading and driving. These cases are often monitored without immediate treatment.
In more advanced cases, the membrane continues to tighten and increases distortion or blur. While macular pucker rarely causes complete loss of vision, prolonged traction can lead to permanent changes in the retinal cells if left untreated.
The decision to treat is based on symptom severity rather than the appearance of the membrane alone. If distortion begins to interfere with quality of life, surgical removal of the membrane can improve clarity and reduce visual distortion.
Can macular pucker heal on its own?
In rare cases, a macular pucker can improve slightly on its own if the scar tissue relaxes. However, most epiretinal membranes do not completely disappear without treatment.
Many macular puckers remain stable for years and cause only mild distortion. If vision is minimally affected, careful observation is often the safest approach. Regular follow-up exams with a retina specialist and retinal imaging help monitor whether the membrane is tightening or progressing.
When the scar tissue continues to contract, vision may become more distorted over time. In those cases, surgical removal of the membrane is the only effective way to correct the problem.
Because spontaneous improvement is uncommon and progression can occur gradually, ongoing monitoring is important to determine the right timing for treatment.
Can macular pucker be corrected?
Yes, macular pucker can be corrected with surgery when symptoms significantly interfere with vision. The procedure, called a vitrectomy with membrane peel, removes the scar tissue that is wrinkling the macula and allows the retina to relax back toward a smoother position.
During surgery, the vitreous gel inside the eye is first removed. The surgeon then carefully peels away the thin epiretinal membrane from the surface of the macula using microscopic instruments. This relieves the traction that is causing distortion.
Surgery is typically recommended only when visual distortion affects reading, driving, or other daily activities. In mild cases, observation is often appropriate because many membranes remain stable for years without progression.
Most patients experience meaningful improvement in distortion after surgery, although some subtle visual changes may persist depending on how long the membrane was present before treatment.
How is macular pucker treated?
Macular pucker is treated based on how much it affects vision. Mild cases that cause minimal distortion are often monitored with regular examinations and retinal imaging. Many patients remain stable for years without needing surgery.
When distortion or blurred central vision begins to interfere with reading, driving, or daily activities, surgery may be recommended. The standard treatment is a procedure called a vitrectomy with membrane peel. During this outpatient surgery, the vitreous gel is removed and the thin scar tissue on the macula is carefully peeled away using microscopic instruments.
The procedure typically takes about 30 minutes and is performed under local anesthesia. Most patients notice gradual improvement in distortion over weeks to months as the macula relaxes and heals. While surgery can improve clarity, it may not completely restore vision if the membrane has been present for a long time.
Your retina specialist will recommend treatment based on the severity of symptoms, retinal imaging findings, and how much the condition is affecting your quality of life.
Where to Get Macular Pucker Treatment in Sarasota and Venice
You can receive expert evaluation and treatment for macular pucker, also known as epiretinal membrane, at any of our Shane Retina locations throughout Sarasota and Venice, Florida. Each office offers advanced retinal imaging, careful monitoring, and surgical treatment options when vision distortion interferes with daily activities.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Our University Parkway location serves patients from Sarasota, Lakewood Ranch, Bradenton, and nearby communities. This office provides comprehensive diagnosis and treatment for macular pucker, including careful monitoring and surgical membrane peel when needed.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our South Tamiami Trail location serves patients throughout Sarasota, Siesta Key, and surrounding neighborhoods. This office offers full evaluation and treatment for macular pucker, with careful surgical planning and postoperative follow up when surgery is required.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Macular Pucker Treatment is Sarasota and Manatee
For more information regarding macular puckers, please visit the American Society of Retina Specialists patient information website: http://www.asrs.org/patients/retinal-diseases/19/epiretinal-membranes.



