Intravitreal Eye Injections in Sarasota, FL
These quick, gentle treatments can help preserve and even improve your vision.
Intravitreal injections deliver medication directly where it’s needed to treat conditions like macular degeneration, diabetic retinopathy, and retinal vein occlusion. Most patients find the procedure fast and comfortable with numbing drops.
If you receive retina care in Sarasota, Bradenton, Lakewood Ranch, or Venice, we offer consultations to determine the right injection plan for you.
Eye Injections and Preventing AMD-related Blindness
An eye injection is done using an ultra-thin needle to deliver medication right to the back of the eye. Eye injections aren’t painful, however, you might feel a little pressure.
At the rear of the eye and the center of the retina lies the macula—the part of the eye that does the high-quality seeing. Most problems of the retina, including age-related macular degeneration (AMD), originate here. Without intravitreal injections, more than 1 million people in the US would lose their central vision—this is the number of people currently living with wet AMD.
What Happens During An Eye Injection?
A retinal ophthalmologist is a specialist qualified to do eye injections. While preparing for the procedure takes a couple of minutes, the actual injection lasts only seconds.
You will lie face up in a comfortable position in a reclining chair. The retina specialist will apply drops in your eyes for numbing. They’ll clean your eyes and eyelids using an antiseptic to reduce the risk of bacterial contamination during the procedure.
After the cleaning, the eye doctor applies an additional anesthetic to your eye using a cotton tip. These numbing eye drops reduce sensation on the eyeball to nearly zero.
The retina specialist then uses a small clip called a speculum to keep your eyelids open during the technique. The specialist will instruct you to look away so he/she can deliver the shot through the white part of your eye.
After the shot, your eye specialist removes the speculum and cleans your eye once again to minimize discomfort. He will further check the eye to ensure there are no complications.
What Are Intravitreal Injections Used For?
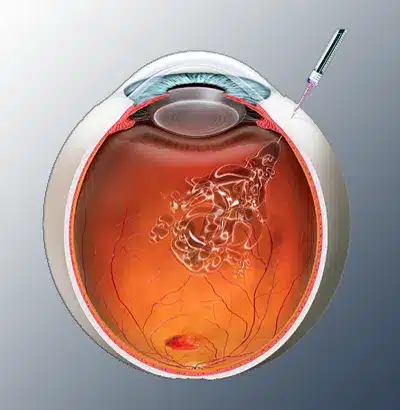
The most common category of medication delivered through the injection is called anti-VEGF. It works for almost all the conditions that cause swelling or bleeding in the retina. The medication stops the growth of abnormal blood vessels, bleeding, and fluid leakage under the retina. A new class of injectable drugs has just gained FDA approval for dry macular degeneration. These medications block a type of immune response in the eye, slowing the formation of blind spots in the central vision. Depending on your eye condition, eye injections might also contain steroid, antibiotic, antifungal, or antiviral drugs.
Eye injections have dependable results in the treatment of many retinal conditions.
Eye Injection Specialist and founder of Shane Retina
How Frequently Should You Have Eye Injections?
Once a retina specialist establishes that you have a condition that would benefit from eye injections, they’ll design a treatment schedule for you.
The frequency of the eye injections depends on the condition, the severity of retinal swelling, and the potency of the medication used. Some can be repeated every 3 months while the most common ones must be administered every 4-6 weeks to maximize the efficiency of the therapy.
In some cases, patients have recovered significant vision as the bleeding stops and retinal swelling improves. Patients with diabetes may need more intermittent shots than other groups of people. The ophthalmologist carefully assesses your condition before deciding that an eye injection is the best approach.
Can Eye Injections Cure Age-Related Macular Degeneration (AMD)?
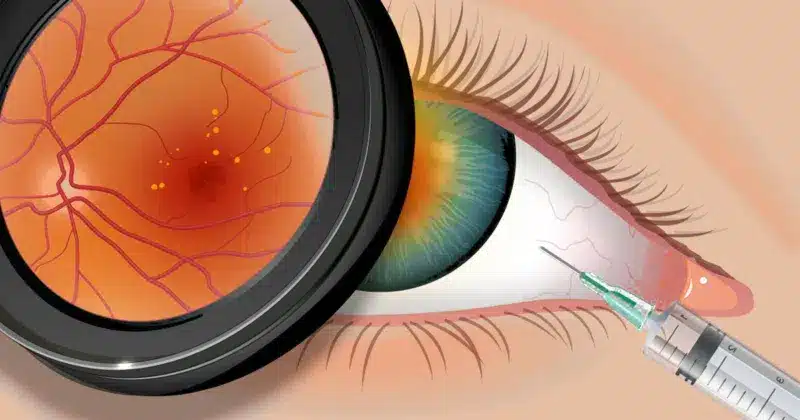
The other type is wet AMD, for which eye injections can also help stop the condition and save vision. Wet AMD is treatable because of its nature—it causes abnormal blood vessels to grow under the retina. They start to leak fluid and blood into the macula. Anti-VEGF medication can stop this.
VEGF is short for vascular endothelial growth factor—this is a protein signal that helps the body to grow new blood vessels when you need them. But when you have AMD, the new blood vessels often tend to be weak and spring up in places that interfere with the eye’s visual acuity. Ant-VEGF medication is delivered via injection to the back of the eye to stop the growth of these troublesome and abnormal blood vessels. As a result, there is less swelling and inflammatory damage to the macula.
How Do Eye Injections Work?
If you are getting the injection for Dry AMD, the shot will contain a complement inhibitor. Currently, the only FDA-approved medication of this kind is pegcetacoplan (Syfovre). Other complement inhibitor medication is expected to gain FDA-approval soon.
Eye injections take some getting used to. It may be scary at first, but the therapy is fast and void of pain. The ophthalmologist does it with great care to keep it minimally invasive.
If you are getting the injection for wet AMD, the shot will contain one of the five anti-VEGF medications:
- Ranibizumab (Lucentis)
- Brolucizumab (Beovu)
- Bevacizumab (Avastin)
- Aflibercept (Eylea)
- Faricimb (Vabysmo)
These meds are all useful in stopping the growth of abnormal blood vessels in the eye. However, they have varying degrees of potency and side effects. The retinal ophthalmologist will consider your medical history before choosing the best option for you.
Intravitreal Eye Injection FAQs
What are eye injections for?
Eye injections are used to deliver medication directly into the back of the eye to treat retinal diseases. They are most commonly used to manage conditions such as wet macular degeneration, diabetic retinopathy, diabetic macular edema, and retinal vein occlusion.
These injections help reduce swelling, stop abnormal blood vessel growth, and prevent further vision loss. In many cases, they can stabilize or even improve vision when given consistently.
By placing medication directly where it is needed, intravitreal injections provide a highly targeted and effective form of treatment.
What is an intravitreal injection?
An intravitreal injection is a procedure in which medication is injected directly into the vitreous cavity, the gel-filled space in the center of the eye. This allows the medication to reach the retina and macula at therapeutic levels.
The word “intravitreal” simply means “inside the vitreous.” By delivering medication directly into the eye, retina specialists can treat conditions such as wet macular degeneration, diabetic retinopathy, retinal vein occlusion, and geographic atrophy more effectively than with pills or eye drops.
The procedure is performed in the office under sterile conditions. The eye is numbed with anesthetic drops, cleaned with antiseptic, and the injection itself takes only a few seconds. Most patients feel pressure rather than pain.
Intravitreal injections are a major advance in modern retina care and have helped prevent vision loss in millions of patients.
Do Eye Injections Work?
Robert Johnson (fictitious name), a Sarasota-based senior, avoided losing his eyesight via early detection and treatment of AMD. During a dilated eye exam, we noticed an increased cluster of drusen in the back of his right eye. We conducted imaging tests that revealed significant swelling in the retina area and confirmed a budding form of wet AMD. Six shots of anti-VEGF within the same year stopped it in its tracks.
Mr. Johnson’s case is just one among the many successful treatments that the ophthalmologists at Shane Retina have had with eye injections. Research continues to search for a way to give injections less frequently or replace them with a topical drop.
Does an Eye Injection Improve Vision?
A good number of patients treated with anti-VEGF have regained normal macular anatomy after consistent treatment. Vision improves as well. However, in patients who have already lost central vision, the medication may not bring back all the vision that was lost.
Do eye injections hurt?
Most patients are surprised to learn that eye injections are not painful. The eye is thoroughly numbed with anesthetic drops before the injection, and many patients feel only mild pressure or slight awareness of the procedure.
The injection itself takes only a few seconds. You may notice brief pressure during the shot, but sharp pain is uncommon. Afterward, the eye can feel slightly scratchy or irritated for the rest of the day, similar to having a grain of sand in the eye. This sensation typically resolves within 24 hours.
Because the procedure is quick and performed under sterile conditions, most patients find it much easier than they expected. Many who were anxious before their first injection report that the experience is far less uncomfortable than anticipated.
Are eye injections safe?
Yes, intravitreal eye injections are considered very safe when performed by a trained retina specialist under sterile conditions. They have been used for over two decades and have prevented vision loss in millions of patients.
The procedure itself is quick and carefully controlled. The eye is cleaned with antiseptic and numbed before the injection to minimize discomfort and reduce the risk of infection.
As with any medical procedure, there are risks, but serious complications are rare. The most serious risk is infection inside the eye, known as endophthalmitis, which occurs in approximately 1 in several thousand injections. Other uncommon risks include retinal detachment or significant inflammation.
More commonly, patients may experience mild redness, irritation, temporary floaters, or slight blurriness for a day or two.
Overall, the risk of not treating conditions like wet macular degeneration is far greater than the risk associated with properly administered eye injections.
How many eye injections will I need?
The number of eye injections you need depends on your specific condition, how severe it is, and how your eye responds to treatment.
Many patients start with a series of monthly injections to control swelling or abnormal blood vessel growth. Once the condition is stable, treatments are often spaced out over time using a “treat-and-extend” approach, where injections are given less frequently while still keeping the disease under control.
Some patients may need ongoing injections every few weeks to months, while others can go longer between treatments. Because retinal conditions are chronic, many people require long-term monitoring and periodic injections to maintain their vision.
Your retina specialist will adjust your treatment plan based on imaging and how your vision responds over time.
What are the side effects of eye injections?
Most side effects of eye injections are mild and temporary. The most common reactions occur on the surface of the eye and typically resolve within a day or two.
Common side effects include:
- Redness on the white part of the eye
- Mild irritation or scratchy sensation
- Temporary blurring of vision
- Small floaters immediately after the injection
- A small surface blood spot where the injection was placed
These symptoms usually improve quickly and do not affect long-term vision.
Rare but serious complications can occur. These include infection inside the eye, known as endophthalmitis, significant inflammation, retinal detachment, or increased eye pressure. Severe pain, worsening vision, or light sensitivity after an injection should be reported immediately.
Although complications are uncommon, retina specialists use sterile technique and careful monitoring to minimize risk. For most patients, the benefits of preventing vision loss far outweigh the potential side effects.
How long do eye injections take to work?
Eye injections start working within days to weeks, but noticeable vision improvement may take several weeks, depending on the condition being treated.
For wet macular degeneration, diabetic macular edema, or retinal vein occlusion, anti-VEGF injections begin reducing retinal swelling shortly after administration. Some patients notice clearer vision within a week or two, while others may require multiple injections before meaningful improvement occurs.
In many cases, the first goal is stabilization rather than immediate improvement. Swelling decreases gradually, and vision may improve over the course of several treatments.
Your retina specialist monitors progress with imaging such as OCT scans to measure changes in retinal fluid and determine how well the medication is working. Treatment intervals may be adjusted based on response.
How long after an eye injection can you drive?
Whether you can drive after an eye injection depends on how your vision feels immediately afterward. Many patients are able to drive the same day, but some prefer to have someone else drive them home.
If your eyes were dilated before the injection, your vision may remain blurry or light-sensitive for several hours. In addition, it is common to experience temporary floaters or mild irritation after the procedure.
For safety, many retina specialists recommend arranging a driver for your first injection so you can see how your eyes respond. If your vision feels clear and comfortable after future injections, you may choose to drive yourself.
Your retina specialist can guide you based on your specific situation and visual stability.
Should I rest after an eye injection?
You do not need strict bed rest after an eye injection, but it is reasonable to take it easy for the rest of the day.
Most patients can resume normal daily activities shortly after the procedure. However, your eye may feel mildly irritated or scratchy for several hours. Avoid rubbing your eye, and follow any post-injection instructions provided by your retina specialist.
It is generally safe to:
- Read or watch television
- Walk around normally
- Perform light household activities
For the first 24 hours, you may want to avoid:
- Heavy lifting
- Strenuous exercise
- Swimming or hot tubs
- Touching or rubbing the eye
If you experience severe pain, worsening vision, or increased light sensitivity, contact your retina specialist immediately.
Can I exercise after an eye injection?
Light activity is usually safe after an eye injection, but strenuous exercise should be avoided for about 24 hours.
You can typically walk, perform normal daily activities, and move around as usual the same day. However, it is best to avoid:
- Heavy lifting
- High-intensity workouts
- Straining or bending repeatedly
- Swimming or hot tubs
Your eye may feel mildly irritated or sensitive for the rest of the day, and avoiding strenuous activity reduces the risk of irritation or increased pressure.
Most patients can return to full exercise the following day unless your retina specialist advises otherwise.
What happens if you stop eye injections for macular degeneration?
Eye injections treat macular degeneration, but they do not cure it. If you stop receiving injections for wet macular degeneration, abnormal blood vessels can begin growing and leaking again.
When this happens, fluid and bleeding can return under the retina. Over weeks to months, this can lead to permanent central vision loss. In many cases, the vision that is lost after stopping treatment cannot be fully recovered, even if injections are restarted later.
That is why consistent treatment is important. Retina specialists often use a treat-and-extend approach to safely lengthen the interval between injections while keeping the disease under control. Stopping treatment entirely without medical guidance increases the risk of irreversible damage.
If scheduling, transportation, or discomfort is making treatment difficult, speak with your retina specialist. Treatment intervals can often be adjusted while still maintaining disease control.
Will Insurance Pay For Eye Injections?
Almost all medical insurances cover the diagnosis and treatment of eye conditions that require eye injections, but you are still subject to their copays, deductibles, and coinsurance. Some insurances will have requirements for which drug is injected into your eye. There are funds sponsored by the drug manufacturers that may help defray some of the cost of the medication.
Where to Get Intravitreal Eye Injections in Sarasota and Venice
You can receive intravitreal eye injections at our Shane Retina locations throughout Sarasota and Venice, Florida. Our ophthalmologists provide ongoing injection therapy for conditions such as macular degeneration, diabetic retinopathy, and retinal vein occlusion, using proven medications to help stabilize and preserve vision.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Our University Parkway location serves patients from Sarasota, Lakewood Ranch, Bradenton, and surrounding areas of Manatee County. This office provides routine intravitreal eye injections for a range of retinal conditions, with efficient visits, careful monitoring, and personalized treatment schedules.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our South Tamiami Trail location serves patients throughout Sarasota, Siesta Key, and nearby Sarasota County communities. Patients at this office receive intravitreal injections as part of long-term treatment plans for retinal disease, with a focus on comfort, consistency, and visual stability.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Patients in Venice, North Port, Englewood, and surrounding areas of southern Sarasota County can receive intravitreal eye injections at this location. Our team provides ongoing injection therapy and follow-up care designed to protect central vision and support daily visual function.
Get Expert Eye Injection Treatment in Sarasota & Venice
If you’ve been told you need eye injections, or you’re noticing changes in your vision, our retina specialists are here to help. We use advanced intravitreal injection therapies to treat macular degeneration, diabetic eye disease, and retinal vein occlusion with a focus on comfort, safety, and long-term results.
Every treatment plan is tailored to your condition, your response to therapy, and your goals for vision. Our team will guide you through each step so you feel confident, informed, and supported throughout your care. You’re in good hands at Shane Retina.



