Retinal Detachment Diagnosis and Emergency Treatment in Sarasota
New flashes, floaters, or a gray curtain in your vision should be checked quickly. Prompt care can help protect your sight.
A retinal detachment is an eye emergency that can lead to permanent vision loss if not treated in time. Most people who notice sudden flashes or floaters do not have a detachment, but there is no way to be sure without a dilated exam.
At Shane Retina, our ophthalmologists offer same-day or next-day appointments to evaluate these symptoms, diagnose retinal tears or detachments, and begin appropriate laser or surgical treatment when needed.
Do I Have a Retinal Detachment?
If you are in this situation, don’t panic but follow this advice before reading the rest of the page. Anyone who is experiencing new flashes and floaters should seek a dilated examination with an ophthalmologist within 24-48 hours. While it is possible that you are in fact experiencing a retinal detachment, the vast majority of patients with these symptoms are not at risk for losing vision. Unfortunately, you cannot be sure that a retinal detachment is not there without an examination by an ophthalmologist.
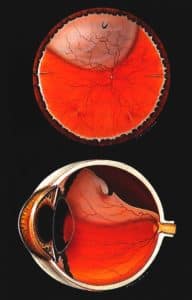
What is the Retina?
The retina is the light-sensitive layer that lines in the inside, back surface of the eye. The light that enters the eye through the pupil passes through the lens to be focused on the retina. The retina interprets the image and passes the signal along the optic nerve to the brain. Without the retina, there would be no vision.
What is a Retinal Detachment?
A retinal detachment (RD) occurs when fluid forms between the retina and its supporting layers in the back of the eye. While there are multiple ways to develop fluid under the retina, the most common reason has to do with the connection between the retina and the jelly that fills the human eyeball.
Throughout your life, the surface of the retina is in contact with the jelly that fills the eye, called the vitreous. Sometime between the ages of 50 and 70 in most people, the jelly spontaneously pulls away from the retina. We call this a posterior vitreous detachment (PVD). This ‘peeling’ of the jelly from the retina puts tension on the retinal surface. This tension is what causes the flashes that are commonly associated with a PVD.
If the jelly pulls hard enough, or the retina has a preexisting area of weakness, a retinal tear can form. A retinal tear occurs in approximately 5% of vitreous jelly separations. The tear can bleed, which is one common reason for new floaters to appear in the vision. While a retinal tear does not directly cause vision loss, it can serve as a pathway for fluid in the eye to travel through the tear and underneath the retina. Think of a retinal tear as a precursor to a retinal detachment.
If fluid from inside the eye does travel through the tear and underneath the retina, a retinal detachment occurs. When the retina becomes separated from it’s supporting layers in the back of the eye, it quickly degenerates and vision loss ensues.
What Our Detached Retina Patients Say
I grew up in Miami where the name Baskin Palmer is golden. Finding Dr. Shane had studied at Baskin was a huge relief. My husband suffered a sudden detached retina so we had no time to waste. Dr Shane changed his schedule at the surgery center, having both the anesthesiologist and the staff stay to accommodate my husband.
The skill and dedication of this man is amazing! It's been a year and a half since the surgery and we are so grateful Sam still has vision in that eye, yes it was that bad of a detachment. Dr. Shane has always been straight forward and explains choices in terms we can understand. We appreciate everything he has done for Sam!!!!!
The staff is also wonderful, so warm and welcoming, and willing to go the extra mile. I work in the healthcare field and know the good side and the bad. Dr. Shane and his staff remain good guys, skilled and knowledgeable, and above all caring and concerned. You are not just a number to them or a 15 minute visit. They care about you!
Did I Cause My Retinal Detachment?
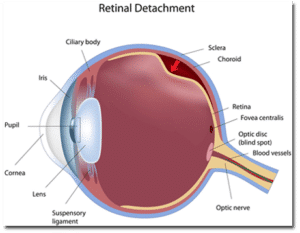
There are a few risk factors, however, that make a retinal detachment more likely. The first would be severe nearsightedness, also known as high myopia. In these patients, the eyeball is much larger than average, with corresponding thinning of the retina. Another risk factor is family history of an RD. Some inherited characteristics that make the jelly or the retina form detachments can be passed down through the generations.
Additional risk factors include previous eye surgery or severe ocular trauma. If you are found to have areas of thinning in your retina, called lattice degeneration or retinoschisis, you may be slightly more likely to develop a retinal detachment. Still, the vast majority of retinal detachments occur for no other reason than the structural limitations of the human eyeball.
The vast majority of retinal detachments occur for no other reason than the structural limitations of the human eyeball.
– Dr. Thomas Shane,
Detached Retina Specialist and founder of Shane Retina
What Happens At My Eye Appointment for New Flashes and Floaters?
If you are experiencing new flashes, floaters, or grey curtain in your vision, you should schedule a dilated eye exam with an ophthalmologist within 24-48 hours. On the day of your appointment, you will have your vision, eye pressure, and peripheral vision checked by a technician. The pupils will be dilated to allow for a clear view of your entire retina. Retinal images will be taken using specialized cameras to detect the presence of a retinal detachment or other eye disease. Lastly, you will be examined by the ophthalmologist and the findings and treatment plan will be discussed.
I Have a Retinal Tear. How Do We Treat It?
If you are found to have a tear in the retina, but no detachment, you will likely undergo a retinal laser to seal the tear and prevent a retinal detachment. The laser works by creating a barrier of scar tissue around the tear, preventing fluid from inside the eye from traveling through the tear and underneath the retina. This procedure can be performed immediately in the office with mild discomfort and no permanent vision loss. Laser for retinal tear typically takes 5 minutes, with patients able to return to their normal activities later in the day.
Keep in mind that it takes at least 7 days for the laser to seal the tear, so you are still at risk for a retinal detachment over than time. In addition, a new tear may form elsewhere in the retina, which can progress to retinal detachment if left untreated. For that reason, it is important to report any onset of new floaters or loss of peripheral vision following your retinal laser.
Important disclaimer: the retinal tear laser is intended to prevent a retinal detachment. Laser for retinal tear does not specifically improve floaters that may be in your vision due to debris suspended in the vitreous jelly that fills the eye. Floater symptoms tend to improve on their own without treatment over the period of weeks and months.
I Have a Retinal Detachment. What Are the Options for Treating It?
Patients found to have retinal detachments should expect to undergo a surgical procedure to repair the problem. There are various options for treating a retinal detachment. The choice of which procedure to use depends on the characteristics of your RD and surgeon preference. Listed below are several options in rough order of least to most invasive.
Retinal Laser: In a minority of cases, a retinal detachment can be isolated with laser alone. The advantage of this treatment is that it can be applied immediately and non-invasively in the clinic. The disadvantage to retinal laser is that it doesn’t prevent progression of the retinal detachment until a week after treatment. For this reason, it is inappropriate for most new retinal detachments, but a reasonable option for those detachments that are chronic in nature.
Pneumatic Retinopexy: This procedure involves the injection of a gas bubble into the eye to flatten the retinal detachment along with laser or freezing treatment to seal the retinal tear. It works well with retinal detachments with single tears located near the top of the eyeball. The advantages to pneumatic retinopexy include that it can be performed same-day in the clinic and leads to slightly better visual outcomes than surgery. The disadvantages include a lower success rate (60-70%) and positioning requirements for ~7 days after the procedure.
Vitrectomy: This outpatient surgical procedure is the most common treatment for all types of retinal detachments. Performed at a hospital or surgery center, it can be accomplished in about 45 minutes using local anesthesia, with a success rate around 85-90%. During the procedure, the surgeon removes the vitreous jelly from the eye, replacing it with clear saline. The retinal is reattached and the tears are lasered from the inside of the eye. A gas or oil bubble is used to hold the retina in place until the laser seals the tears. Patients frequently have to take uncomfortable head positions for 7 days and avoid air travel for weeks following a vitrectomy for retinal detachment.
Scleral buckle: This outpatient surgical procedure was one of the first solutions to retinal detachments, dating back to the 1950’s. Success rates for scleral buckle are similar to vitrectomy, but require larger incisions and carry an increased risk for double vision and nearsightedness afterwards. On the other hand, the risk for cataract is much lower for scleral buckle than vitrectomy. For this reason, scleral buckle tends to be the procedure of choice for patients who develop retinal detachments before the age of 50.
How Soon Do We Treat a Retinal Detachment?
Most retinal detachments require some form of surgical repair within 1-2 weeks. The urgency of the repair depends on the extent of the detachment. If the separation of the retina has not yet progressed through the center of the vision (macula-on), the surgeon may schedule a procedure within 24-48 hours depending on surgery center availability. If the retinal detachment has already involved the central vision, then the timing of the procedure is usually 1-7 days after diagnosis with comparable visual outcomes.
Retinal Detachment FAQs
What is retinal detachment?
Retinal detachment occurs when the retina separates from the back wall of the eye, cutting off its blood and oxygen supply. If not treated promptly, this separation can lead to permanent vision loss.
The retina is the light-sensitive layer that allows you to see. In most cases, a retinal detachment begins with a retinal tear. Fluid from inside the eye then passes through the tear and collects underneath the retina, lifting it away from its normal position.
Retinal detachment is considered an eye emergency. Early diagnosis and treatment improve the chances of preserving vision.
What are the symptoms of a detached retina?
The most common symptoms of a retinal detachment include sudden flashes of light, new or increased floaters, and a dark shadow or “curtain” moving across part of your vision.
Patients may notice:
- Sudden flashes, like lightning streaks in the side vision
- A shower of new floaters or black spots
- A gray shadow or curtain coming from the side
- Blurry or distorted peripheral vision
- Sudden loss of part of the visual field
Retinal detachment usually does not cause pain. The vision changes happen because the retina is lifting away from its normal position and can no longer process light correctly.
If you experience any combination of new flashes, floaters, or a curtain in your vision, you should seek a prompt dilated eye examination. These symptoms often appear suddenly and require urgent evaluation.
How can you tell if you have a retinal detachment?
You cannot reliably tell on your own if you have a retinal detachment without a dilated eye examination. While certain warning signs strongly suggest a detachment, only a retina specialist can confirm the diagnosis.
Common warning signs include:
- A sudden increase in floaters
- Repeated flashes of light
- A gray or dark curtain moving across your vision
- Sudden loss of peripheral vision
- Rapidly worsening blur in one eye
These symptoms occur when the retina begins to lift away from the back of the eye. However, flashes and floaters alone do not always mean a detachment is present. Many people experience similar symptoms during normal vitreous separation.
The only way to know for certain is through a prompt dilated exam, where the entire retina can be carefully evaluated. If you are experiencing new flashes, floaters, or a shadow in your vision, you should be examined as soon as possible to rule out a retinal tear or detachment.
What causes retinal detachment?
Retinal detachment is most commonly caused by a retinal tear that allows fluid to pass underneath the retina and lift it away from the back of the eye. The tear usually develops when the vitreous gel inside the eye shrinks and pulls on the retina.
As we age, the vitreous naturally separates from the retina in a process called posterior vitreous detachment. In most people, this occurs without complication. However, if the vitreous pulls hard enough on a weak area of the retina, it can create a tear. Once a tear forms, fluid can seep underneath and cause the retina to detach.
Certain risk factors increase the likelihood of retinal detachment, including:
- High nearsightedness
- Previous retinal detachment in the other eye
- Family history of retinal detachment
- Eye trauma
- Prior eye surgery
- Areas of retinal thinning such as lattice degeneration
In many cases, retinal detachment occurs due to the natural structural changes of the eye rather than anything the patient did. Prompt treatment of retinal tears can often prevent progression to a full detachment.
Does a detached retina hurt?
No, a detached retina usually does not cause pain. Most patients experience sudden changes in vision rather than discomfort.
Retinal detachment occurs when the retina lifts away from the back of the eye, but the retina itself does not have pain receptors. Instead of pain, patients typically notice flashes of light, new floaters, or a dark curtain or shadow in their vision.
Because there is no pain, some people delay seeking care, assuming the symptoms will improve. This delay can increase the risk of permanent vision loss.
Any sudden change in vision, even without pain, should be treated as urgent and evaluated promptly with a dilated eye examination.
How is retinal detachment treated?
Retinal detachment is treated with procedures designed to reattach the retina and seal any tears. The specific treatment depends on the size, location, and severity of the detachment, as well as whether the central vision has been affected.
If only a retinal tear is present and the retina is still attached, a laser or freezing treatment can often seal the tear and prevent detachment.
Once a detachment has occurred, surgical repair is usually required. The most common treatment options include:
- Pneumatic retinopexy, which involves placing a gas bubble inside the eye to press the retina back into position
- Vitrectomy, a surgical procedure that removes the vitreous gel and reattaches the retina from inside the eye
- Scleral buckle, a procedure that places a supportive band around the eye to relieve traction on the retina
These procedures are typically performed in an outpatient surgical center. The urgency of treatment depends on whether the macula, the center of vision, is still attached. Early intervention improves the likelihood of preserving vision.
Can a detached retina heal on its own?
No, a detached retina will not heal on its own. Once the retina separates from the back wall of the eye, it cannot reattach without medical or surgical treatment.
When the retina is lifted away, its blood and oxygen supply are disrupted. Without prompt repair, the light-sensitive cells begin to lose function and can suffer permanent damage. The longer the retina remains detached, the greater the risk of irreversible vision loss.
In rare cases, very small areas of detachment may appear stable for a short period, but they do not spontaneously reattach. Surgical intervention is required to reposition the retina and seal any tears.
Because timing is critical, anyone experiencing symptoms of retinal detachment should seek immediate evaluation. Early treatment offers the best chance of preserving useful vision.
Can a detached retina be fixed?
Yes, a detached retina can often be successfully repaired with prompt surgical treatment. Modern techniques allow retina specialists to reattach the retina and preserve or restore vision in many cases.
The type of repair depends on the size and location of the detachment. Common procedures include vitrectomy, pneumatic retinopexy, or scleral buckle surgery. All are designed to reposition the retina against the back of the eye and seal the tear that caused the detachment.
The outcome depends heavily on timing. If the macula, the center of vision, is still attached at the time of surgery, the chances of maintaining excellent vision are high. If the macula has already detached, surgery can still reattach the retina, but full visual recovery may be limited.
Early evaluation and treatment by a retina specialist offer the best chance of a successful outcome. Retinal detachment is serious, but with modern surgical care, it is often fixable.
How long before retinal detachment causes blindness?
Retinal detachment can begin causing permanent vision damage within hours to days, particularly if the macula is involved. The retina depends on a constant blood supply, and once it is separated from the back of the eye, the light-sensitive cells begin to lose function quickly.
If the detachment has not yet reached the macula, central vision may still be preserved. In these cases, surgery is often performed urgently, sometimes within 24 to 48 hours, to prevent permanent central vision loss.
If the macula has already detached, the situation is still urgent, but the timeline for irreversible damage has already begun. While surgery can successfully reattach the retina, the longer the macula remains detached, the less likely full visual recovery becomes.
Retinal detachment does not typically cause immediate complete blindness, but delaying treatment significantly increases the risk of permanent and severe vision loss. Any symptoms suggestive of detachment should be evaluated by an ophthalmologist as soon as possible.
How long can retinal detachment go untreated?
Retinal detachment should not be left untreated. The longer the retina remains detached, the higher the risk of permanent and irreversible vision loss. In some cases, significant damage can begin within days, especially if the macula becomes involved.
If the detachment has not yet affected the macula, central vision may still be preserved, but this window can close quickly. Once the macula detaches, visual recovery becomes less predictable, even after successful surgery. Weeks of untreated detachment can result in severe and lasting vision impairment in many cases.
In addition to vision loss, prolonged detachment can lead to scarring and contraction of retinal tissue, making surgical repair more complex and reducing the likelihood of full visual recovery.
Because timing is critical, any symptoms such as flashes, new floaters, or a curtain in the vision should prompt immediate evaluation. Early diagnosis and treatment provide the best chance of preserving sight.
Where to Get Emergency Retinal Detachment Evaluation and Treatment in Sarasota and Venice
You can receive urgent evaluation and treatment for retinal detachment at our Shane Retina locations throughout Sarasota and Venice, Florida. Our ophthalmologists offer same day or next day appointments to diagnose retinal tears or detachments and begin appropriate laser or surgical treatment to help preserve vision.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Patients experiencing new flashes, floaters, or sudden changes in vision can receive prompt evaluation for retinal detachment at our office on University Blvd in North Sarasota near Lakewood Ranch. Our team provides urgent diagnostic imaging and immediate treatment planning, including in office laser or referral for same day surgical repair when necessary.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our office on South Tamiami Trail offers rapid evaluation for retinal detachment and retinal tears in patients with sudden vision symptoms. Our ophthalmologists are experienced in managing eye emergencies and can initiate laser treatment or arrange urgent surgical care to help prevent permanent vision loss.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Patients with sudden flashes, floaters, or a gray curtain in their vision can receive urgent evaluation for retinal detachment at our office in Venice, Florida. Our team performs same day diagnostic testing and coordinates timely laser or surgical treatment when needed to protect vision.
Retinal Detachment Reviews
Just a little over a year ago Dr Gabriel performed the bubble procedure to address a detached retina. Today after seeing my retina specialist in Huntsville AL, we all agree that Gabriel did a great job.
It was truly a blessing finding you while vacationing in Venice.
Over New Year’s 2025 I feared I had a detached retina. I called my ophthalmologist’s office but there was no one there and was referred to Shane Retina. They called me back quickly and got me in at 8am the next day. I was amazed at that!
Dr. Shane and his staff then conducted a very thorough exam with advanced machinery and explained my condition…thankfully NOT a detached retina! I can’t say enough good things about this office and the service they provide.
Contact Us in Sarasota or Manatee County for Retinal Detachment Symptoms
Have you been experiencing new flashes of light, floaters, or sudden loss of vision? You may have a retinal detachment. We offer emergency retinal detachment surgery or laser treatments in Sarasota & Manatee County.
Our ophthalmologists located in Sarasota and Manatee County is specialized in managing retinal detachments. A retinal detachment is considered an eye emergency, and permanent vision loss is possible if treatment is delayed. If you are having the symptoms mentioned above, seek a prompt dilated eye examination with our practice immediately. There are effective surgical and clinical treatments for most retinal detachments, so don’t delay.



