Retinal Tear Treatment in Sarasota, FL
Early treatment of a retinal tear can often prevent a retinal detachment and protect your vision.
A retinal tear occurs when the gel inside the eye pulls on the retina, sometimes causing sudden flashes, new floaters, or a shadow in your vision. A prompt dilated exam is the only way to confirm whether a tear is present and determine if laser or freezing treatment is needed.
If you are experiencing new flashes, floaters, or blurred areas in one eye in Sarasota, Bradenton, Lakewood Ranch, or Venice, we offer prompt appointments to evaluate and treat possible retinal tears.
Retinal Tear Treatment
The retina is the inner lining of the eyeball which senses light and sends these light signals to the brain to be interpreted as vision. Think of the retina like the wallpaper of your eyeball and the pupil as the window to let light into the room. For various reasons, people can develop retinal tears in this very thin tissue that could result in permanent loss of vision. The following information is designed to help guide you through the various causes and types of retinal tears and subsequent retinal tear treatment solution performed by retina specialists.
Causes Of A Retinal Tear
The traditional rhegmatogenous retinal tear is created when the vitreous humor (the “jelly” that fills the eye) separates from the retinal surface. This is known as a Posterior Vitreous Detachment (PVD). The vitreous will often start its separation in the center of the eye (at the optic nerve and macula) and progress out to the peripheral retinal where the vitreous originates. When the vitreous pulls on the peripheral retinal (which is significantly thinner than the central retina)–a retinal tear can occur. Some individuals who have lattice (thin spots in the peripheral retina) have an increased risk of a retinal tear and detachment when the vitreous humor separates.
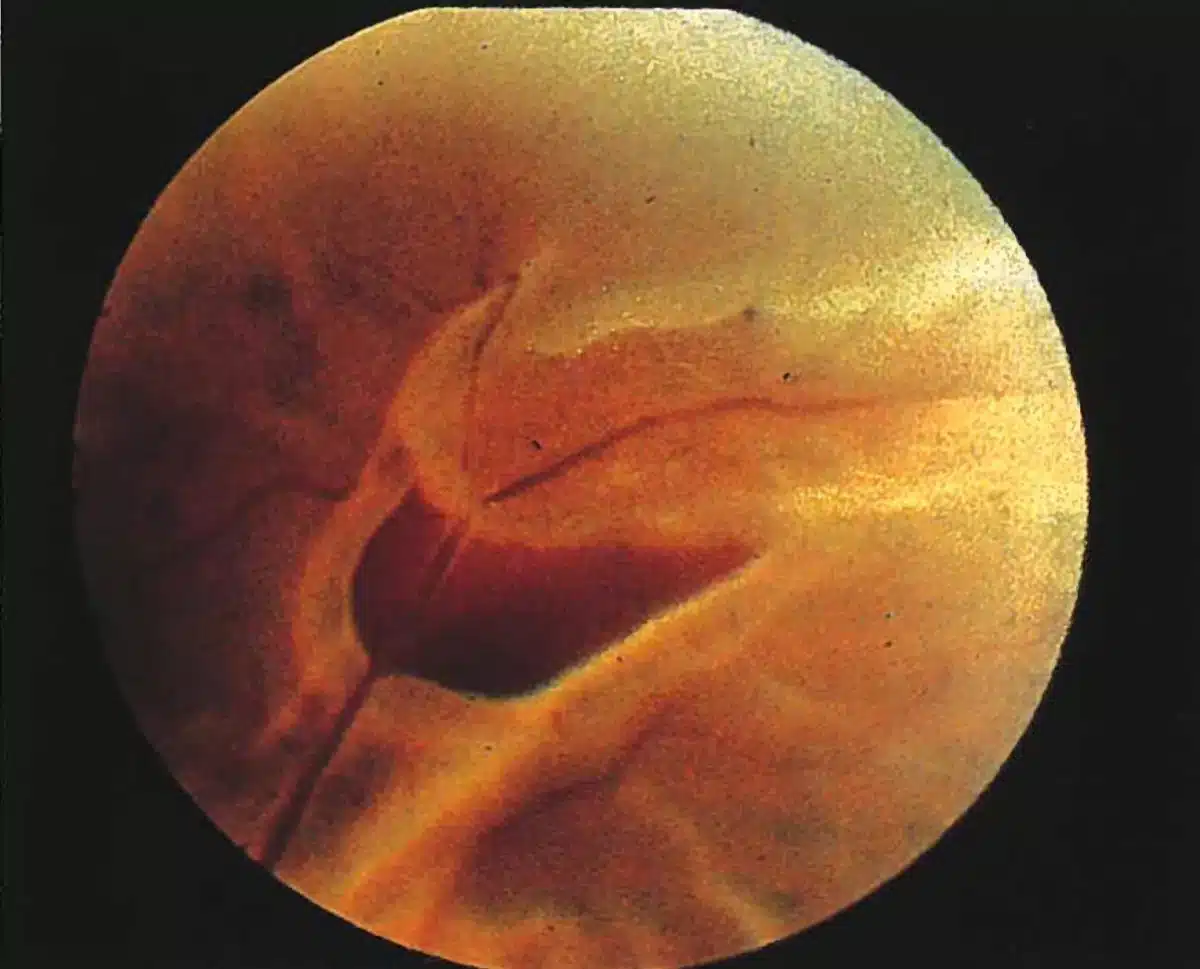
A tear in the retina can be categorized based on its appearance during a clinical exam by an ophthalmologist. There are three main types of retinal tears: an operculated tear (small circle of tissue torn out of the retina), a horseshoe tear (a ‘U’-shaped flap is lifted up), or a Giant Retinal Tear (a tear involving greater than 25% of the retina).
Risk Factors for Retinal Tear
- Severe nearsightedness
- Pre-existing thinning of the retina called lattice degeneration
- Prior eye surgery
- Advanced Age
- Trauma to the eyeball
- Previous Retinal Tear in the Other Eye
Symptoms Of A Retinal Tear
A retinal tear has similar symptoms of those with a posterior vitreous detachment. As the vitreous separates from the retina, it can cause a variety of symptoms, including new flashes or floaters. A retinal tear also causes flashes and floaters, and is indistinguishable from a vitreous detachment without a dilated examination. In a percentage of patients, there will be no symptoms and retinal tears may be discovered during routine examination by ophthalmologists. The following are a more detailed description of the common symptoms of PVDs/retinal tears:
Floaters – Patients may experience an increase in floaters–both large and small. The large floater is sometimes referred to as a Weiss Ring which is a piece of collagen that has pulled off from around the optic nerve giving it a ring appearance. Also, patients may perceive many small black dots sometimes described as black pepper flakes in the eye. These tiny floaters can be blood or pigment cells that have been released from the retina when a tear is present. Only a careful dilated eye examination can determine the origin and cause of the floaters.
Flashes of Light – The retina is a neurosensory tissue designated to sense light and send those signals to the brain. When physically irritated by traction from the jelly in the eye, the retina will send false signals of light to the brain. The patient will perceive flashing light or “lightning bolts” in their vision. These flashes can be blamed on the normal, spontaneous separation of the vitreous jelly as it peels off of the retina or possibly a retinal tear. Either way, when a patient is experiencing new flashes of light, the best way to determine if there is a retinal tear or detachment is to have an ophthalmologist perform a dilated exam of the peripheral retina.
Curtain of Blurred Vision – If a retinal tear has formed, ocular fluid can begin to migrate through the retinal tear and under the retina causing a retinal detachment. These detachments will originate in the peripheral retina and are often not visually significant. However, as more fluid accumulates under the retina propagating the detachment, patients will notice a dark curtain of blurred vision opposite of where the retina is detaching. These symptoms require urgent examination to determine the cause of the loss of vision before retinal tear treatment.
Complications Of A Retinal Tear
Over time, the vitreous jelly that fills the eye becomes less like jelly and more like water. During this degradation, the vitreous can peel off of the retina and cause tears. Subsequently, the water that fills the eye can go through the tear and under the retina causing a retinal detachment. Referring back to the previous analogy, the eye is like a fluid-filled room with the retina being like the wallpaper in the room. If a tear existed in the wallpaper, fluid could seep underneath it. If enough water got underneath the wallpaper, it would start to peel off and detach. The same is true for the retina. Early recognition of a tear and prompt retinal tear treatment can prevent a large retinal detachment requiring invasive surgical repair.
Treatment Of A Retinal Tear
If identified early, a retinal tear can be treated with an in-office procedure. The two mainstay treatments for retinal tear are laser and freezing (cryopexy).
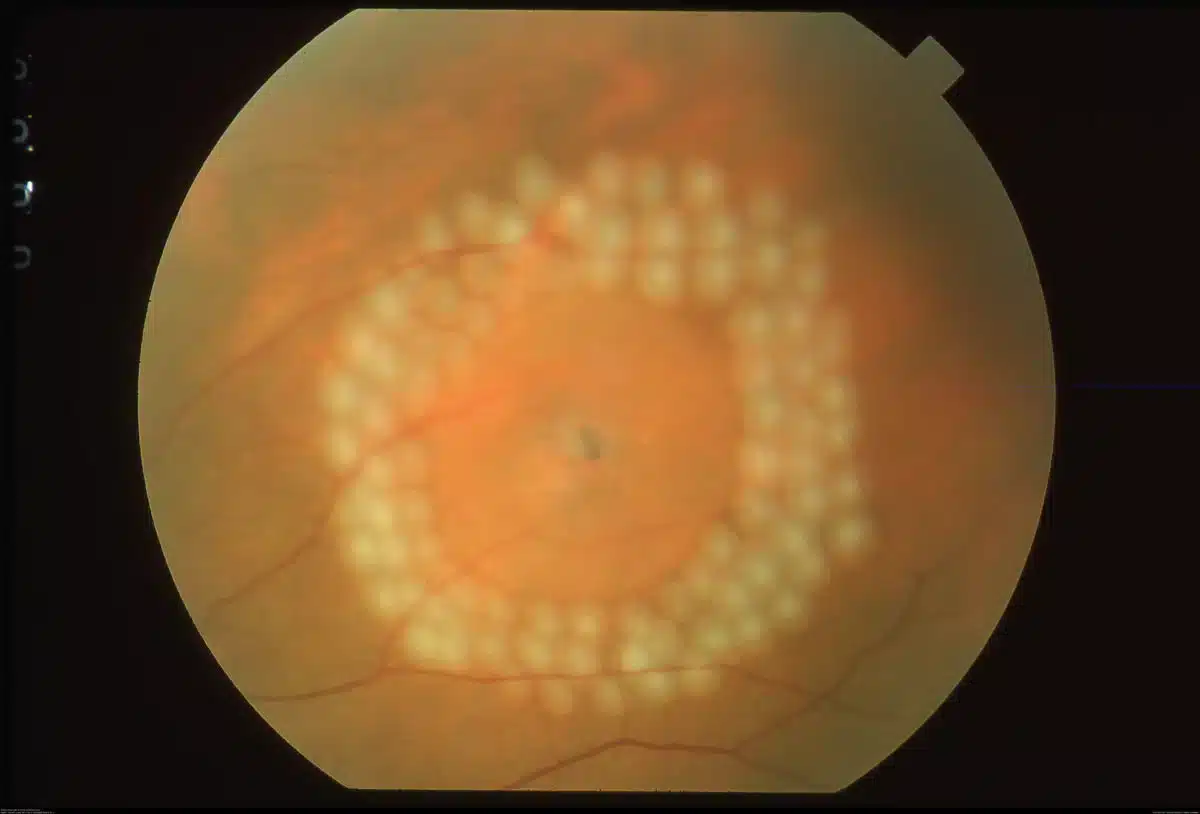
Laser: The retina can be treated to seal the borders around a retinal tear using a laser. The laser energy is absorbed by the retina, creating a tiny burn that scars the retinal layers together. This “weld” prevents any fluid from passing through the retinal tear and under the retina. The laser creates an adherence of the retinal layers that will be ultimately healed in 1-2 weeks. Laser cannot be successfully used if the retina is already detached, which is why surgery is usually the preferred treatment for retinal detachment.
Freezing (Cryopexy): Using a specialized probe, the retina specialist will freeze the tissue through the eye wall, creating inflammation and eventually scarring of the tissue to close the retinal tear. Similar to laser, freezing treatment results in no immediate adherence of the retina and will take time for the healing process to finalize. This can be an uncomfortable process, and some clinicians will elect to perform a numbing injection prior to treatment.
Note that both of these techniques can be used with attached retina. If there is fluid under the retina (a retinal detachment), the laser or freezing can be applied in combination with other procedures to attach the retina simultaneously. To reattach the retina in the office, a gas bubble is injected into the eye and placed over the retinal tear by having the patient position their head for 1-3 days. The fluid under the retina will be absorbed through natural retinal fluid pumps. Thereafter, the retina can be treated with laser or freezing. If there is a very large or complex retinal detachment, surgery is then recommended to reattach the retina and then apply laser at the same time.
Retinal Tear FAQs
What causes a retinal tear?
A retinal tear is most commonly caused by age-related separation of the vitreous gel from the retina, a process called posterior vitreous detachment. As the gel shrinks and pulls away, it can tug on thin or weakened areas of the peripheral retina and create a tear.
Most vitreous detachments are harmless, but in a small percentage of cases, the pulling force is strong enough to cause a tear. If fluid passes through that tear, it can lead to a retinal detachment.
Certain factors increase the risk of a retinal tear, including severe nearsightedness, lattice degeneration, previous eye surgery, prior retinal tears, and eye trauma. However, many retinal tears occur simply as part of normal aging.
What is the most common cause of a retinal tear?
The most common cause of a retinal tear is age-related posterior vitreous detachment, when the vitreous gel shrinks and pulls on thin areas of the peripheral retina.
This process typically occurs between ages 50 and 70 and is part of normal aging. While most vitreous detachments are harmless, in some cases the traction is strong enough to cause a tear.
What are the symptoms of a retinal tear?
The most common symptoms of a retinal tear are the sudden appearance of new floaters or flashes of light. Many patients describe seeing small dark specks, cobwebs, or black pepper-like dots in their vision. Flashes may appear as brief streaks of light in the side vision, especially in dim lighting.
Some patients may also notice a shadow or gray curtain in their peripheral vision. This can signal that fluid is beginning to pass through the tear and may indicate early retinal detachment.
Retinal tears are painless. Because the symptoms can be subtle but serious, any sudden increase in floaters, flashes, or loss of side vision should prompt urgent evaluation with a dilated eye examination.
Does a retinal tear hurt?
No, a retinal tear does not hurt. The retina does not contain pain receptors, so even though a tear can threaten vision, it typically causes no physical discomfort.
Instead of pain, patients usually experience visual symptoms such as sudden flashes of light or new floaters. Because there is no pain warning signal, retinal tears can sometimes be overlooked.
That is why any sudden change in floaters, flashes, or peripheral vision should be evaluated promptly with a dilated eye exam. Early detection allows treatment before a retinal detachment develops.
Can a retinal tear heal on its own?
Most retinal tears do not reliably heal on their own. While a small tear may sometimes remain stable for a period of time, there is no dependable way to predict whether it will progress.
The concern is not the tear itself, but what can happen afterward. If fluid passes through the tear and spreads underneath the retina, it can lead to a retinal detachment, which is a much more serious condition requiring surgery.
Because of this risk, retinal tears are usually treated with laser or freezing therapy to create a protective scar barrier around the tear. This greatly reduces the risk of retinal detachment.
Prompt treatment is far safer than waiting to see whether a tear will remain stable.
How can you tell if you have a retinal tear?
You cannot confirm a retinal tear without a dilated eye examination. The symptoms of a retinal tear can feel similar to a normal vitreous separation, so only a retina specialist can determine whether a tear is present.
Warning signs may include:
- A sudden increase in floaters
- Flashes of light in the side vision
- New dark spots that look like pepper flakes
- A shadow or gray curtain in the peripheral vision
However, some retinal tears cause no symptoms at all and are discovered during routine exams.
Because there is no reliable way to tell the difference at home, any sudden change in floaters, flashes, or peripheral vision should be evaluated within 24 to 48 hours by a retina specialist. Early detection allows simple in-office treatment before a retinal detachment develops.
Can a retinal tear cause blindness?
Yes, a retinal tear can lead to blindness if it progresses to a retinal detachment and is not treated promptly.
A tear by itself does not usually cause permanent vision loss. However, if fluid passes through the tear and lifts the retina away from the back of the eye, the light-sensitive cells can become permanently damaged. This is called a retinal detachment.
The risk of blindness increases if the detachment reaches the central retina, known as the macula. Once the macula is involved, visual recovery may be limited even after surgery.
The good news is that when a retinal tear is detected early, simple in-office laser treatment can substantially reduce the risk of detachment and help preserve vision.
How is a retinal tear treated?
A retinal tear is usually treated with a quick in-office procedure designed to seal the tear and prevent a retinal detachment. The two most common treatments are laser retinopexy and cryotherapy.
Laser treatment creates a small ring of scar tissue around the tear. This scar forms a barrier that prevents fluid from passing underneath the retina. The procedure takes only a few minutes and is performed under numbing drops.
In some cases, freezing treatment, called cryopexy, is used instead of laser. This also creates scar tissue that seals the tear in place.
If a tear is treated early, these procedures are very effective at preventing retinal detachment. Prompt treatment greatly reduces the risk of more invasive surgery and helps preserve long-term vision.
What should I expect after laser surgery for a retinal tear?
Laser treatment for a retinal tear is performed in the office and usually takes only a few minutes. The goal of the laser is to create a small scar around the tear that seals it and prevents fluid from passing underneath the retina.
During the procedure, you may see bright flashes of light and feel mild pressure, but it is generally well tolerated.
After treatment, you may notice:
- Mild irritation or scratchiness
- Light sensitivity
- Temporary blurring
- Slight increase in floaters
These symptoms typically improve within a day or two.
It takes about one to two weeks for the laser scar to fully seal the tear. During that time, it is important to report any new flashes, floaters, or loss of peripheral vision, as new tears can occasionally form elsewhere.
Most patients can return to normal daily activities the same day, although your retina specialist may advise avoiding strenuous activity briefly.
Can you fly after laser surgery for a retinal tear?
Yes, in most cases you can safely fly after laser treatment for a retinal tear.
Laser therapy alone does not place a gas bubble inside the eye, so there are no altitude-related restrictions. Commercial air travel does not affect the laser scar that is forming around the tear.
However, if a gas bubble was placed in the eye as part of treatment for a retinal detachment or combined procedure, flying is strictly prohibited until the bubble has completely dissolved. Changes in cabin pressure can cause the gas bubble to expand, which can dangerously increase eye pressure.
Your retina specialist will confirm whether a gas bubble was used and whether it is safe for you to fly.
Where to Get Retinal Tear Evaluation and Treatment in Sarasota and Venice
You can receive prompt evaluation and treatment for retinal tears at our Shane Retina locations throughout Sarasota and Venice, Florida. Our ophthalmologists diagnose retinal tears with dilated examination and provide in-office laser or freezing treatment when appropriate to help prevent retinal detachment and protect vision.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Our University Parkway location serves patients from Sarasota, Lakewood Ranch, Bradenton, and surrounding areas of Manatee County. This office provides prompt evaluation for retinal tears and offers same-day laser or cryopexy treatment when needed to reduce the risk of progression to retinal detachment.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our South Tamiami Trail location serves patients throughout Sarasota, Siesta Key, and nearby Sarasota County communities. Patients at this office receive timely diagnosis and treatment for retinal tears, including in-office laser or freezing procedures designed to seal the tear and preserve vision.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Patients in Venice, North Port, Englewood, and surrounding areas of southern Sarasota County can receive evaluation and treatment for retinal tears at this location. Our team provides careful examination and prompt treatment to help prevent retinal detachment and avoid more invasive surgical repair.
Get Treatment For a Retinal Tear
Retinal tears may not be common in the general public, however, they are common enough to keep retina specialists busy. Holes in the retina need to be appropriately identified and treated in a timely manner. The retina specialists at Shane Retina are trained to identify retinal tears and detachments and administer office lasers, gas bubbles, and sometimes surgery the same day. If you are experiencing new floaters, flashing lights, or blurred vision, please make an appointment with your retinal specialist.