Macular Hole Diagnosis and Surgery in Sarasota & Manatee County, FL
A new blind spot or distortion in one eye can be frightening. Macular hole surgery often restores useful vision.
A macular hole is a small gap in the very center of the retina that can cause a missing spot or distortion in your central vision. It does not usually cause pain, but it can make reading, driving, or recognizing faces much more difficult.
At Shane Retina, our ophthalmologists specialize in macular hole diagnosis and surgery, offering high closure rates and carefully guided recovery to help you regain as much clarity as possible.
What Is the Macula?
The macula is the center of the retina and is responsible for sharp vision. It lies along the back inside surface of the eye. The light that enters the eye through the pupil is focused by the lens onto the macula. The macula then interprets the light and sends the information along the optic nerve to the brain.
The center of the macula, called the fovea, is the one-millimeter area where vision is sharp enough to read newspaper print. To reduce interference with vision, the inner layers of the retina are pushed aside within the fovea, allowing light to strike directly on the photoreceptors. This creates the normal appearance of a dip in the center of the macula.
On the surface of the macula lies the vitreous jelly that fills the eye. The vitreous jelly is in contact with the surface of the retina for the first 50-70 years of life, but slowly begins to separate throughout middle age. It is the separation of the vitreous jelly that begins the process of macular hole formation in some patients.
What Causes A Macular Hole?
A macular hole occurs when centrifugal forces on the surface of the retina pull the macula apart directly in the center of the vision. The forces that pull on the retina most commonly stem from the vitreous jelly tugging on the macula as it naturally separates from the retina with age. Membranes on the surface of the retina may also contribute to the forces pulling the macula apart.
In almost every case, there is nothing the patient did to cause a macular hole. While severe eye trauma can cause macular holes, most head or eye injuries do not result in this condition. Nutrition or general overall health also do not contribute. On the other hand, a person is certainly at elevated risk for macular hole if they have experienced one in their other eye. Similarly, there may be an inherited risk for macular hole if a close relative has also had the condition.
What Are the Symptoms of Macular Hole?
A macular hole typically results in a painless blind spot in the center of vision in one eye. The hole may go unnoticed if it is not located in the person’s dominant reading eye. However, with the good eye covered, most patients will complain of a missing spot in the center of a word on the page. Occasionally, a patient will only experience distortion without the blind spot.
What Should I Do If I Have A Blind Spot or Distortion in One Eye?
Anyone with new distortion or blurry vision in one eye should seek a dilated examination with an ophthalmologist. On the day of your visit, you will have your vision tested, eye pressure checked, and pupils dilated. Retinal imaging will then be performed to capture an image of the gap in your central retina. Afterwards, the ophthalmologist will examine your eyes and discuss the findings and recommended treatments with you.
What Is the Most Popular Treatment Option for Macular Hole?
In most cases, a macular hole will not close without treatment. In fact, the longer a hole can exist, the less likely that it will close with treatment. Do not panic however…closure rates of macular holes are still >95% in most cases, even with months of delay prior to treatment.
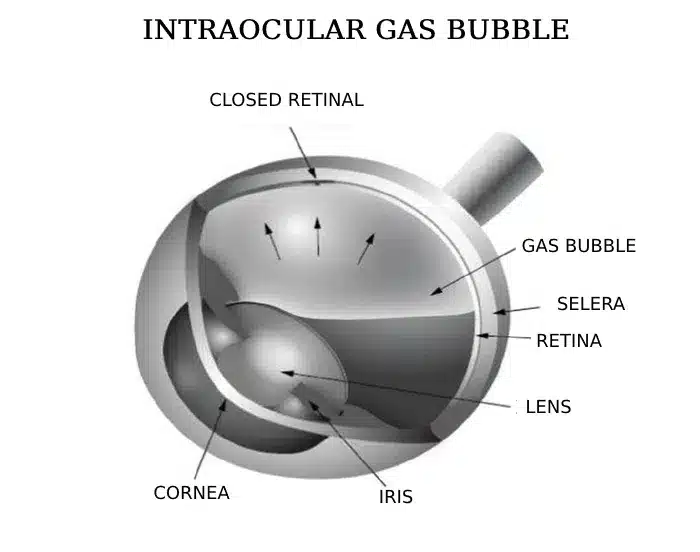
The most common method for closing a macular hole is with surgery. This typically takes place in an ambulatory surgery center under local anesthesia, like a cataract surgery. The surgery lasts around 45 minutes and involves removing the vitreous jelly from inside the eye, called a vitrectomy. Next, a membrane is peeled form the surface of the macula to relieve any persistent tractional forces around the edge of the hole. Then the eye is filled with a bubble of gas, which helps draw the edges of the hole back together again.
After surgery, the patient is typically required to spend several days in face-down positioning. The allows the gas bubble to press directly on the hole, increasing the chances for successful closure. Unfortunately, the vision is not good while the gas bubble is in the eye, typically for the period of two weeks. However, once the bubble is reabsorbed by the body, the hole is found to be closed and vision improved in greater than 95% of cases.
Despite the high success of surgery, patients should be aware of the risks and side effects. Besides the discomfort of face down positioning and temporary blurring of vision, patients may also experience a progression of their cataracts in the months after surgery. Vitrectomy carries a 2% risk for retinal detachment in the weeks and months following macular hole repair. Lastly, patients are restricted from flying while the gas bubble is in the eye.
Are There Any Other Treatments for Macular Hole?
While surgery is the most successful treatment for all macular holes, patients may achieve successful closure through less invasive means. One such treatment involves the injection of a gas bubble into the eye in the clinic, called a pneumatic vitreolysis. By pushing on the vitreous jelly, the bubble can break the connection between the jelly and the edges of the hole, which may relieve enough traction around the hole to allow it to close.
Some macular holes are so small that they respond to eye drops. These drops are designed to dehydrate the retina, which is sometimes enough to draw the edges of the macular hole back together. This treatment only works for a significant minority of macular holes (<5%).
Do Macular Holes Reopen? What Then?
Sometime a macular hole will not close with treatment or reopen months or years later. The risk factors for unsuccessful closure include the size of the hole, how long it was present before treatment, and whether a full retinal membrane peel was performed at the time of surgery. Fortunately, the rate of macular hole recurrence is less than 5% in most studies.
If a macular hole is persistent, the only real treatment option is to return to surgery. The surgeon can perform additional surgical maneuvers that were not done in the first surgery, including enlarging the retinal membrane peel, using a longer acting gas bubble, and increasing the time in face-down positioning.
Retinal surgeons worldwide continue to explore new ways to close persistent macular holes. Several new techniques have been proposed, including placing tissue over the hole, physically pushing/pulling the edges of the macular hole together, and using retinal incisions to relax the tension on the macular surface. While each method reports some success, it is yet unknown which will prove the most effective and easiest to perform.
Macular Hole FAQs
What is a macular hole?
A macular hole is a small opening that forms in the center of the retina, in the area called the macula that controls sharp central vision. This gap can cause a blurry or missing spot in the center of your vision.
The macula allows you to read, drive, and recognize faces. When a hole develops in this area, the light-sensitive cells are pulled apart, disrupting how visual information is processed. Most macular holes occur as part of the natural aging process when the vitreous gel inside the eye shrinks and pulls on the retinal surface.
Macular holes typically affect one eye and do not cause pain. However, they can significantly interfere with daily activities if left untreated.
What causes a macular hole?
A macular hole is most commonly caused by age-related changes in the vitreous gel inside the eye. As the vitreous naturally shrinks and separates from the retina over time, it can pull on the center of the macula. If the traction is strong enough, it can create a small opening in the retinal tissue.
This process typically occurs between the ages of 50 and 70 and is not something patients cause through lifestyle or activity. In most cases, macular holes develop spontaneously as part of normal aging.
Less commonly, macular holes can result from eye trauma, high nearsightedness, previous retinal surgery, or the presence of scar tissue on the retinal surface. Patients who have had a macular hole in one eye are also at increased risk of developing one in the other eye.
Surgical treatment is highly effective in closing most macular holes, especially when addressed promptly.
What are the symptoms of a macular hole?
The most common symptom of a macular hole is a blurry or distorted spot in the center of vision in one eye. Straight lines may appear bent or wavy, and small details such as letters in a word may look missing.
Patients often notice:
- A dark or gray spot in the center of vision
- Difficulty reading fine print
- Distortion of straight lines
- Trouble recognizing faces
- A sensation that objects appear smaller or slightly misshapen
Because the condition usually affects only one eye, it can go unnoticed at first if the other eye sees well. Covering one eye at a time can help reveal subtle changes.
Macular holes do not cause pain, redness, or flashing lights. Any new central distortion or blind spot should be evaluated promptly by an ophthalmologist, as earlier treatment generally leads to better visual outcomes.
Can a macular hole heal itself?
In rare cases, a very small macular hole can close on its own, but most full-thickness macular holes do not heal without treatment. Spontaneous closure is uncommon and usually occurs only in early or very small defects.
Because a macular hole forms when traction pulls the retinal tissue apart, those forces often continue unless treated. Over time, the hole may enlarge, leading to worsening central vision.
For this reason, careful monitoring with retinal imaging is important. If the hole is small and vision remains relatively stable, short-term observation may be reasonable. However, when vision declines or the hole progresses, surgery is typically recommended.
Modern macular hole surgery has a high success rate in closing the hole and improving vision, especially when performed before long-standing retinal damage develops.
Can a macular hole be repaired and how is it treated?
Yes, a macular hole can usually be repaired with surgery. The most effective treatment is a procedure called a vitrectomy with membrane peel.
During surgery, the vitreous gel that is pulling on the macula is carefully removed. The surgeon then peels away any microscopic membranes on the surface of the retina that are contributing to traction. A small gas bubble is placed inside the eye to gently press the edges of the hole together while it heals.
The procedure is performed in an outpatient surgical center under local anesthesia. Most surgeries take less than an hour. Over the following weeks, the hole gradually closes as the retinal tissue heals.
In select cases involving very small holes, less invasive treatments such as a gas injection in the office may be considered. However, surgery remains the most reliable method for achieving closure and restoring central vision.
Prompt evaluation is important if a macular hole is suspected.
How long is recovery after macular hole surgery?
Recovery after macular hole surgery typically takes several weeks, although vision can continue to improve gradually for up to six to twelve months. The first few days focus on healing and protecting the eye, while vision gradually improves over time.
Immediately after surgery, a gas bubble is placed inside the eye to help the hole close. Because of this bubble, vision will be very blurry at first and may look like you are seeing through water. As the gas bubble gradually dissolves over several weeks, vision begins to clear.
Some patients are instructed to maintain specific head positioning for several days after surgery to help the hole seal properly. Your surgeon will provide detailed guidance if positioning is required.
Most patients are able to resume light daily activities within a few days, but strenuous activity should be avoided until cleared by your retina specialist. While many patients experience meaningful improvement in distortion and central clarity, final visual results depend on how long the hole was present before surgery.
Can I sleep on my side after macular hole surgery?
Whether you can sleep on your side after macular hole surgery depends on your surgeon’s specific instructions and whether a gas bubble was placed in your eye. In many cases, patients are asked to maintain a certain head position for several days to help the hole close properly.
The gas bubble acts like a gentle internal bandage, pressing against the macula to encourage healing. Depending on the location of the hole, you may be instructed to position face-down or avoid certain positions while sleeping. These positioning requirements are usually temporary and clearly explained before and after surgery.
After the initial healing period, most patients can gradually return to normal sleeping positions. It is important to follow your retina specialist’s guidance closely, as proper positioning can significantly improve the chances of successful hole closure.
Can I drive after macular hole surgery?
Most patients cannot drive immediately after macular hole surgery, especially while a gas bubble is still present in the eye. Vision is often significantly blurred during this time, making driving unsafe.
The gas bubble placed during surgery gradually dissolves over several weeks. Until it fully disappears and vision stabilizes, depth perception and clarity may be reduced. If only one eye was operated on, you may rely on the other eye for vision, but this should be discussed with your retina specialist before driving.
In general, patients can consider returning to driving once the gas bubble has resolved, vision has improved, and they meet legal visual requirements. Your surgeon will evaluate your healing and advise you on when it is safe to resume driving.
Safety should always come first. Even if you feel comfortable, confirm with your ophthalmologist that your vision meets legal driving requirements.
Where to Get Macular Hole Surgery in Sarasota and Venice
You can receive expert macular hole diagnosis and surgical treatment at any of our Shane Retina locations throughout Sarasota and Venice, Florida. Each office provides advanced retinal imaging, surgical evaluation, and proven macular hole repair options focused on restoring central vision and guiding recovery safely.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Our University Parkway location serves patients from Sarasota, Lakewood Ranch, Bradenton, and nearby communities. This office provides comprehensive diagnosis and surgical treatment for macular holes, including vitrectomy and advanced macular repair techniques.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our South Tamiami Trail location serves patients throughout Sarasota, Siesta Key, and surrounding neighborhoods. This office offers full evaluation and surgical management of macular holes, with careful preoperative planning and postoperative guidance.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Our Venice Retina location serves patients in Venice, North Port, Englewood, and nearby communities. This office provides evaluation and surgical treatment for macular holes, including vitrectomy when indicated.
Macular Hole Specialists in Sarasota and Manatee
At Shane Retina, we are experts at problems involving the macula, including macular hole surgery. If you have developed this condition or think you need macular hole surgery in Sarasota or Manatee county, we can help. Call us to set up a dilated eye examination this week with one of our experienced ophthalmologists. This exam may involve photographs or other specialized imaging tests of the retina. There are effective surgical treatments for macular holes, so do not delay your evaluation.
Contact us today for more information regarding macular holes or macular hole surgery in Sarasota, FL, and Manatee County. You can also visit the American Academy of Ophthalmology patient information website or the American Society of Retina Specialists patient information website: http://www.asrs.org/patients/retinal-diseases/4/macular-hole.