Macular Edema Diagnosis and Treatment in Sarasota, FL
Swelling in the macula can blur your central vision. Early, targeted treatment can help restore clarity.
Macular edema is swelling in the central part of the retina that can cause painless, often frustrating blurriness in one or both eyes. It can occur with conditions like macular degeneration, diabetes, retinal vein occlusion, eye surgery, or inflammation inside the eye.
At Shane Retina, our ophthalmologists specialize in identifying the exact cause of macular edema and tailoring treatment to protect and improve your vision.
Macular Edema Symptoms and Diagnosis
Macular degeneration is not the only retinal condition that threatens central vision with age. In fact, there are many reasons for swelling to show up in the macula, and it takes an ophthalmologist specialized in retina to determine the cause and recommend the correct treatment. Shane Retina is specialized in diagnosing and treating the many causes for macular edema in Sarasota and Manatee Counties.
What Is the Macula?
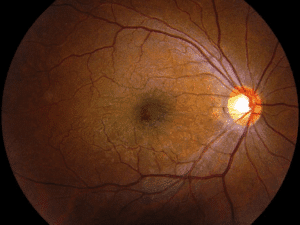
The retina is a thin structure that lines the inside back surface of your eyeball. The entire surface of the retina is around two square inches. The central 5% of the retina, where vision is sharpest, is called the macula. Light enters the eye through the pupil and is focused by the lens onto the macula to create reading and driving vision.
What Is Macular Edema?
Macular edema is another word for macular swelling. Macular edema comes from leaky blood vessels that course below, above, or within the retinal layers. On a microscopic level, abnormal retinal blood vessel walls allow fluid to pass from the bloodstream into the retina, distorting the normal retinal architecture.
There are many causes for macular edema. In most cases, the retina is injured, inflamed, infected, or experiencing low blood flow. These mechanisms lead to the release of chemical signals that modify the integrity of the blood vessel walls. Interestingly, while the blood vessels allow fluid to escape, the gaps in the vessel walls are not typically large enough to allow for bleeding.
What Retinal Conditions Lead to Macular Edema?
The most common conditions that lead to macular edema are macular degeneration, diabetic retinopathy, and retinal vein occlusion. There are other common, but less well-known causes for macular edema, including hypertension, cataract surgery inflammation and uveitis. With these three conditions, the swelling that occurs is called cystoid macular edema (CME).
When a patient experiences extended periods of extremely high blood pressure, the retinal vessels can leak fluid. This would be analogous to the leakage that would occur if an old garden hose were put under too much water pressure. Sometimes the blood vessel wall protrudes, called a macroaneurysm.
CME is one of the most frequent side effects of eye surgery, particularly cataract surgery. Ophthalmologists currently believe that this retinal leakage occurs due to post-surgical inflammation that causes macular vessels to leak. It typically appears a few weeks following cataract extraction, notable to the patient as an unexplained worsening of central vision. Up to 50% of patients experience cystoid macular edema after cataract surgery, but only a handful require extended treatment by a retina specialist. In most cases, CME resolves over time with or without treatment.
Another cause for cystoid macular edema is uveitis, a generic term for inflammation in the eye. There are many countless reasons for an eye to be inflamed, but most fall under the category of infections or autoimmune conditions, where the body’s immune system attacks its own tissue. Uveitis is a complex process requiring lab work-up and other specialized testing to determine the proper diagnosis and treatment.
Rarely, cystoid macular edema can occur without infection or inflammation. This so called ‘non-leaking’ CME may be due to inherited retinal disorders, epiretinal membranes, or too much vitamin (niacin) supplementation.
What Are the Symptoms of Macular Edema?
Macular edema causes painless blurring of central vision in one or both eyes. In some cases, the eye may be red or sensitive to light. The symptoms may fluctuate over time. Macular edema does not cause transient loss of vision, double vision, or eye irritation. The condition may be associated with a history of autoimmune disease or recent eye surgery.
How Is Macular Edema Diagnosed?
If the ophthalmologist is unsure of the source of the macular edema, he may order additional images with a camera technology called fluorescein angiography. This test involves injecting dye into an arm vein and taking pictures at it flows through the retinal vessels. Any swelling withing the macula glows brighter as the test progresses, sometimes revealing the source of the leakage.
Anyone who suspects that they may have macular edema should seek a dilated exam with an ophthalmologist, preferably one specialized in macular and retinal conditions. During your appointment, your vision will be checked, and eyes dilated. Specialized images of your retina using optical coherence tomography (OCT) will be obtained. Then the ophthalmologist will examine your eyes with a lighted microscope before discussing diagnostic and treatment options with you.
If there is inflammation in the eye, the eye doctor may order lab testing to look for common infections or autoimmune conditions that manifest in the eye.
How Is Macular Edema Treated?
Correctly diagnosing the underlying cause for macular edema is critical to instituting the appropriate treatment. For macular degeneration, injections of medication are first choice. Hypertension, diabetic retinopathy, and retinal vein occlusion also benefit from injections, but in conjunction with blood sugar and blood pressure control.
When cystoid macular edema occurs after cataract surgery, the first-line therapy involves drops of steroid and ibuprofen-like medication. If these treatments are found to be insufficient, steroids can be injected directly into the eye. Typically, the need for these therapies goes down over time.
When uveitis (eye inflammation) is the main cause for retinal swelling, steroid drops are commonly the initial treatment until lab results come back. Depending on the infection or autoimmune condition that is identified, a patient may be treated with antibiotics, antivirals, steroid injections, oral steroids, or even steroid-sparing immune suppressants. Sometimes, a rheumatologist is consulted for management of any systemic medications.
What Are the Side Effects of Treatment for Macular Edema?
The goal of treatment for macular edema is to restore vision without otherwise harming the eye. The various treatments mentioned previously are all considered safe, but the ophthalmologist will be on the lookout for well-known side effects.
Some prescription drops can become irritating to the eye or cause a surface allergy. When steroid medication is used to treat macular swelling, eye pressure can become temporarily elevated. These patients may have to be treated with pressure-lowering drops and watched for the onset of glaucoma. For eye injections, there is a 1/5000 risk for infection, which can be blinding.
When systemic immune suppressants or steroids are used, a whole host of familiar side effects are possible. Anyone who takes oral or injectable medications for macular edema should be followed in consultation with their primary care doctor or rheumatologist.
What Are the Outcomes After Treatment of Macular Edema?
Most patients successfully rid themselves of retinal swelling with the appropriate treatment and time. Even those who are not able to eliminate their macular edema are able to stabilize their vision with ongoing treatment.
Macular Edema FAQs
What is macular edema?
Macular edema is swelling in the macula, the part of the retina responsible for sharp central vision. It occurs when fluid leaks from small blood vessels into the retinal tissue, causing blurry or distorted central vision.
The macula allows you to read, drive, and recognize faces clearly. When fluid accumulates within its layers, the normally smooth retinal structure becomes thickened and distorted. This interferes with how light is processed, leading to painless central blurring.
Macular edema is not a disease by itself but a complication of other retinal conditions such as diabetic retinopathy, retinal vein occlusion, macular degeneration, inflammation inside the eye, or recent eye surgery.
Early treatment is important because prolonged swelling can damage the retinal cells responsible for central vision.
What causes macular edema?
Macular edema is caused by leakage from damaged or inflamed blood vessels in the retina. When the walls of these tiny vessels become weak, fluid escapes into the macula and leads to swelling that blurs central vision.
The most common causes of macular edema include:
- Diabetic retinopathy
- Retinal vein occlusion
- Age-related macular degeneration
- Inflammation inside the eye, known as uveitis
- Recent eye surgery, especially cataract surgery
In diabetes and vein occlusions, poor blood flow and vessel damage make the retinal vessels more likely to leak. In inflammatory conditions, chemical signals released in the eye increase vessel permeability. After cataract surgery, temporary inflammation can sometimes lead to a specific type called cystoid macular edema.
Because macular edema is usually a complication of another retinal condition, identifying the underlying cause is essential. Treatment focuses on reducing the swelling while controlling the condition that triggered it.
What are the symptoms of macular edema?
The most common symptom of macular edema is painless blurring of central vision. Objects may appear distorted, washed out, or less sharp than usual, especially when reading or focusing on fine detail.
Patients often report:
- Blurry or fuzzy central vision
- Wavy or distorted straight lines
- Difficulty reading small print
- Colors appearing dull or faded
- A gray or dark spot in the center of vision
Vision changes may develop gradually or fluctuate depending on the cause. In some cases, especially when inflammation is present, the eye may feel mildly light-sensitive or appear slightly red.
Because macular edema affects the central retina, peripheral vision usually remains normal. However, if swelling persists without treatment, permanent damage to the macula can occur. Prompt evaluation with retinal imaging is important to identify the cause and begin treatment.
Is macular edema serious and can it cause vision loss?
Yes, macular edema can be serious because it affects the central part of the retina responsible for sharp vision. If left untreated, persistent swelling can damage the light-sensitive cells in the macula and lead to permanent central vision loss.
The severity depends on the cause and how long the swelling has been present. Mild cases may cause only subtle blurring, while more significant edema can interfere with reading, driving, and recognizing faces. The longer fluid remains in the macula, the greater the risk of lasting retinal damage.
The encouraging news is that many forms of macular edema respond to modern treatments such as eye injections, anti-inflammatory medications, or laser therapy, depending on the underlying condition. Early diagnosis and targeted treatment improve the chances of stabilizing or restoring vision.
Can macular edema go away on its own?
In some cases, macular edema can improve on its own, but this depends entirely on the underlying cause. Mild swelling after cataract surgery, known as cystoid macular edema, often resolves gradually with time or with short-term use of anti-inflammatory drops.
However, macular edema caused by diabetes, retinal vein occlusion, or macular degeneration usually does not resolve without treatment. In these cases, ongoing leakage from damaged blood vessels continues to cause swelling until the underlying condition is addressed.
Because it is impossible to determine the cause of macular swelling without proper imaging and examination, any new central blurring should be evaluated promptly by an ophthalmologist. Early treatment improves the chance of visual recovery and reduces the risk of permanent retinal damage.
How is macular edema treated?
Macular edema is treated by reducing retinal swelling while controlling the condition that caused it.
For swelling caused by diabetic retinopathy or retinal vein occlusion, anti-VEGF eye injections are often the first line of treatment. These medications reduce leakage from abnormal blood vessels and can significantly improve or stabilize central vision. In some cases, steroid injections may also be used to decrease inflammation.
When macular edema occurs after cataract surgery, anti-inflammatory eye drops are usually prescribed first. If swelling persists, steroid injections may be considered. If inflammation inside the eye is the cause, treatment may include steroid drops, oral medications, or immune-modulating therapy depending on the diagnosis.
Successful treatment depends on accurately identifying the underlying condition. With early and appropriate therapy, many patients experience meaningful improvement in vision or stabilization of the disease.
What is cystoid macular edema?
Cystoid macular edema, often abbreviated as CME, is a specific type of macular swelling in which fluid collects in small, cyst-like spaces within the layers of the macula. These tiny pockets of fluid cause the retina to thicken and distort, leading to blurry or wavy central vision.
CME commonly occurs after eye surgery, especially cataract surgery, due to temporary inflammation inside the eye. It can also develop in association with uveitis, retinal vein occlusion, diabetic retinopathy, or other inflammatory conditions.
In many post-surgical cases, cystoid macular edema improves with anti-inflammatory eye drops over several weeks. More persistent cases may require steroid injections or other targeted treatments. Because CME can resemble other retinal conditions, specialized imaging such as OCT is used to confirm the diagnosis and guide treatment.
What is diabetic macular edema?
Diabetic macular edema, often called DME, is a complication of diabetic retinopathy in which fluid leaks into the macula and causes swelling in the center of the retina. This swelling blurs central vision and is one of the most common causes of vision loss in people with diabetes.
Over time, elevated blood sugar damages the small blood vessels in the retina. When these vessels become weak, they leak fluid into the surrounding retinal tissue. When this leakage affects the macula, reading and recognizing faces can become difficult.
Diabetic macular edema may develop gradually and sometimes causes only mild symptoms at first. Without treatment, however, prolonged swelling can lead to permanent central vision loss.
The most common treatment for diabetic macular edema involves anti-VEGF eye injections, which reduce leakage and swelling. With early diagnosis by a retina specialist and consistent treatment, many patients are able to stabilize and sometimes improve their vision.
Your Shane Retina Care Team
Macular edema is diagnosed and treated at Shane Retina by our team of fellowship-trained retina specialists. Our physicians use advanced imaging to detect the swelling that causes macular edema and develop a treatment plan to reduce it and protect your central vision.

Thomas Shane, M.D.

Anita Shane, M.D.

Konica Singla, M.D.

Maria Castaños, M.D.

Gabriel Dib, FNP-C

Ayah Etyem, PA-C
Where to Get Macular Edema Treatment in Sarasota and Venice
You can receive expert evaluation and treatment for macular edema at any of our Shane Retina locations throughout Sarasota and Venice, Florida. Each office provides advanced diagnostic imaging and proven treatment options for macular edema and diabetic macular edema, focused on reducing retinal swelling and preserving central vision.
Sarasota - University Parkway Office
Located just west of I-75 on University Parkway in University Health Park.
Our University Parkway location serves patients from Sarasota, Lakewood Ranch, Bradenton, and nearby communities. This office provides comprehensive evaluation and treatment for macular edema, including care for diabetic macular edema and other retinal swelling conditions.
Sarasota - South Tamiami Trail Office
Located on South Tamiami Trail just south of Bee Ridge Road.
Our South Tamiami Trail location serves patients throughout Sarasota, Siesta Key, and surrounding neighborhoods. This office offers full diagnosis and treatment for macular edema, with access to advanced imaging and injection-based therapies when indicated.
Venice Retina Office
Located in central Venice near Venetia Bay Boulevard.
Our Venice Retina location serves patients in Venice, North Port, Englewood, and nearby communities. This office provides evaluation and treatment for macular edema for patients in Venice and surrounding communities.
Your Macular Edema Specialists in Sarasota And Manatee
Shane Retina, is specialized in managing macular edema. If you experience the symptoms mentioned above, consider having a dilated eye examination with an ophthalmologist. This exam may involve photographs or other specialized imaging tests of the retina. There are effective treatments for macular edema, so do not delay your evaluation.
For more information regarding age-related macular degeneration, please visit the American Society of Retina Specialists patient information website: http://www.asrs.org/patients/retinal-diseases/20/macular-edema or click on links to articles written by our retina specialists below.



